Scar Formation After Surgery: Why Some Scars Heal Better Than Others
Dr. Mohan Rangaswamy
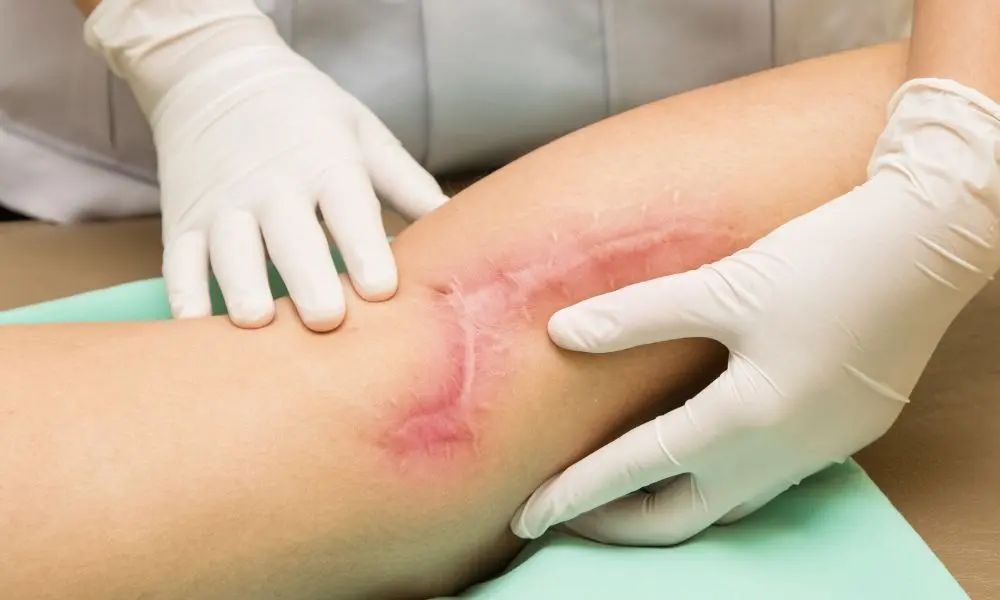
Scar formation after surgery is one of the most common concerns patients have before undergoing any procedure. While surgery is often performed to restore function, correct deformity, or improve appearance, the quality of scar healing plays a major role in long-term satisfaction. Patients frequently ask why some scars fade quietly into the skin while others remain raised, pigmented, or noticeable long after healing is complete.
The truth is that scar formation after surgery is influenced by a complex interaction of biological factors, surgical technique, wound care, and individual healing responses. Scars are not merely a result of the incision itself; they reflect how the body repairs tissue and how thoughtfully the procedure was planned and executed.
In experienced surgical practice, scar management begins long before the first incision is made. Dr. Mohan Rangaswamy approaches every procedure with careful consideration of tissue handling, incision placement, and healing dynamics, aiming to achieve functional success while minimizing long-term scar visibility.
Understanding Scar Formation After Surgery
Scar formation after surgery is a natural part of the body’s healing process. When the skin is cut, the body produces collagen fibers to repair the wound. These fibers form a scar, which gradually remodels over time.
The healing process occurs in stages:
- Inflammation: The body responds immediately to injury, increasing blood flow and immune activity.
- Proliferation: New tissue and collagen begin forming to close the wound.
- Maturation: Collagen reorganizes, and the scar gradually softens and flattens.
While this process follows the same biological principles in everyone, the final appearance of a scar can vary significantly from person to person.
Why Some Scars Heal Better Than Others
Not all scars are equal. Several factors determine why scar formation after surgery results in subtle lines for some patients and more noticeable scars for others.
1. Individual Healing Biology
Genetics play a powerful role in scar formation. Some individuals naturally produce more collagen or heal with thicker scar tissue. Generally speaking, persons of North European origin (Fitzpatrick type 1)generally form good fine scars while persons of African origin or from far east (Fitzpatrick type 6) tend to form thicker scars Others may be prone to hypertrophic scars or keloids due to inherited tendencies.
Skin type, pigmentation, and age also influence healing. Younger skin tends to heal faster but may produce more robust scarring, while older skin heals more slowly but often with finer scars.
2. Location of the Surgical Incision
Different areas of the body heal differently. Areas under constant movement or tension—such as the chest, shoulders, abdomen, or joints—are more likely to develop prominent scars.
Experienced surgeons account for these factors by placing incisions along natural skin lines and areas of reduced tension whenever possible. This strategic planning significantly affects long-term scar quality.
3. Surgical Technique and Tissue Handling
One of the most critical determinants of scar formation after surgery is how the procedure is performed. Gentle tissue handling, precise incision placement, minimal trauma, and meticulous closure all contribute to better scar outcomes.
Dr. Mohan Rangaswamy emphasizes surgical precision and respect for tissue planes. By minimizing unnecessary trauma and ensuring accurate alignment during closure, the healing process is optimized from the outset.
The Role of Surgical Planning in Scar Outcomes
Scar management does not begin after surgery—it begins during planning.
Incision Placement Strategy
Well-planned incisions follow natural creases, folds, or anatomical landmarks. When scars align with these natural lines, they tend to blend more seamlessly with surrounding skin.
Layered Closure Techniques
Closing the wound in layers reduces tension on the skin surface. This approach allows deeper tissues to absorb stress, preventing excessive pulling on the scar itself.
Dr. Mohan’s approach focuses on layered closure and long-term stability rather than simply closing the skin. This philosophy plays a vital role in minimizing widened or thickened scars.
Types of Scars That Can Form After Surgery
Understanding different scar types helps patients set realistic expectations.
Fine-Line Scars
These are flat, pale scars that fade over time and often become barely noticeable.
Hypertrophic Scars
Raised, thick scars that remain within the boundaries of the original incision.
Keloid Scars
Overgrown scar tissue extending beyond the incision line, often associated with genetic predisposition.
Pigmented Scars
Scars that appear darker or lighter than surrounding skin due to melanin changes.
Experienced surgeons assess risk factors for these scar types during consultation and adjust surgical plans accordingly.
Postoperative Care and Its Impact on Scar Formation After Surgery
Even with excellent surgical technique, postoperative care plays a crucial role in scar quality.
Wound Care Compliance
Proper cleaning, dressing changes, and infection prevention are essential in early healing.
Sun Protection
Exposure to UV radiation can darken scars permanently. Protecting healing scars from sunlight is critical.
Scar Modulation Therapies
Silicone gels, pressure therapy, and massage can improve scar texture and appearance when used appropriately.
Patients under Dr. Mohan’s care receive clear, individualized guidance on postoperative scar care to support optimal healing.
Why Experience Matters in Scar Management
Scar formation after surgery is not only about the incision—it is about anticipating healing behavior and adapting technique accordingly.
With over three decades of surgical experience, Dr. Mohan Rangaswamy has managed a wide spectrum of procedures, from reconstructive surgeries to aesthetic corrections. This depth of experience allows for:
- Anticipation of high-risk scarring
- Adjusted incision strategies
- Proactive scar prevention measures
- Long-term follow-up and refinement
Experience brings perspective—knowing when subtle adjustments make a significant difference months or years later.
Psychological Impact of Scars and Patient Expectations
Scars are not just physical marks; they can affect confidence, self-image, and emotional well-being.
An important part of surgical care involves setting realistic expectations. No surgery is completely scar-free, but thoughtful planning and execution can ensure scars are as discreet and acceptable as possible.
Dr. Mohan prioritizes transparent patient education, helping individuals understand what to expect and how healing evolves over time.
When Scar Revision May Be Considered
In some cases, scars may heal unpredictably despite best practices. Scar revision procedures may be considered when scars:
- Cause functional restriction
- Remain painful or inflamed
- Are disproportionately noticeable
Scar revision is not merely cosmetic—it requires careful timing, assessment of scar maturity, and precise technique to avoid recurrence.
How Dr. Mohan Approaches Scar Minimization
Scar minimization is not a single step but a continuous process that includes:
- Preoperative risk assessment
- Strategic incision planning
- Gentle surgical technique
- Meticulous wound closure
- Structured postoperative care
Dr. Mohan Rangaswamy’s approach focuses on achieving the primary surgical goal while respecting the body’s natural healing processes. This balance is key to long-term outcomes that patients can feel comfortable with. Dr. Mohan uses the following treatment techniques for scar minimization:
- Fractional laser
- Microneedling
- Careful use of steroid injections
- Nanofat grafting
Common Myths About Scar Formation After Surgery
“Smaller incisions always mean smaller scars”
Not necessarily. Tension, location, and healing response matter more than incision length alone.
“Scars stop changing after a few weeks”
Scar maturation can take up to a year or longer.
“All scars can be erased”
Scars can be improved, not erased. Honest counseling is essential.
Long-Term Healing: What Patients Should Know
Scar formation after surgery continues to evolve long after visible healing appears complete. Over months, collagen remodels, redness fades, and texture softens. Patience, adherence to care instructions, and regular follow-up are essential components of successful healing.
Final Thoughts: Scar Formation Is a Shared Responsibility
Scar formation after surgery reflects a partnership between surgical expertise and patient care. While biology cannot be controlled entirely, thoughtful planning, refined technique, and informed postoperative care can significantly influence outcomes.
Dr. Mohan Rangaswamy’s practice emphasizes precision, safety, and long-term results over short-term appearance. By respecting both the science of healing and the individuality of each patient, his approach aims to deliver outcomes that heal well—not just immediately, but for years to come.